
A data-driven service designed to improve collaboration, workflow efficiency, and MRI protocols. With Clinical Advisory Services supporting continuous improvement efforts, the MR Department of Máxima MC is able to quickly identify workflow challenges and successfully define and deploy improvement solutions for the MR fleet.

Clinical Advisory Services consist of three phases: Current state assessment, Solution design, and Performance management. Maxima MC and Philips have teamed up to run through all phases to assess, define and achieve their goals
To maintain a high standard of care amid increasing competition and growing demand, the MRI imaging department must focus on improving patient throughput, reducing waiting times, and maximizing scanner utilization. Having a central platform to monitor key performance indicators (KPIs) and identify outliers in these areas, while receiving ongoing support throughout your continuous improvement journey, is the essential first step toward achieving lasting performance gains.
This article describes a collaboration between Philips and Máxima Medisch Centrum to gather and assess quantitative and qualitative data, identify areas of improvement, implement a plan, and assess the results.
At the public facility Máxima Medisch Centrum (Máxima MC), the Medical Imaging department staff is dedicated to continuous performance improvement. The site incorporated the Philips Clinical Advisory Service, including performance analytics tools and advisory consultation, to gain insights on the performance of their three MR systems.
Using a data-driven decision-making process, coupled with advisory support, they identified inefficiencies and streamlined their processes, improving throughput and patient care.
In 2024 and 2025, Philips partnered with Máxima MC to assess and optimize the performance of its MRI department. The goal of the collaboration was to improve image quality, workflow efficiency, and interdepartmental communication. The project evolved from a pilot into a catalyst for sustainable improvement, combining data-driven insights with hands-on clinical engagement.
The Clinical Advisory Services engagement followed a structured methodology consisting of three phases:
A. Current State Assessment: Through data gathering, which included MR system data analysis, staff surveys, and interviews bottlenecks and improvement areas were identified. Quantitative data was collected from Philips systems, while qualitative insights were gathered through interviews and on-site observations.
B. Solution Design: The solution was designed in collaborative workshops and protocol optimization sessions.
C. Performance Management: In this phase, implementation was tracked, follow-up reviews were conducted, and continuous improvement was planned.
Philips acted as a catalyst. With their guidance, we were able to optimize the image quality in MSK— essential for better diagnostics.

In the first phase of the project, the Philips team and the Máxima MC MR team conducted a current state assessment. Quantitative data was collected from the system log files and presented using data analytics dashboards, understanding the MR department’s performance looking at different aspects of the MR examination process such as procedure time, changeover time, software utilization, protocol variation.
The teams concluded that the protocols and study durations were standardized and performed without many outliers or variability in the protocols used or the duration of the exams. The software utilization and adoption were found to be on par with local benchmarks.
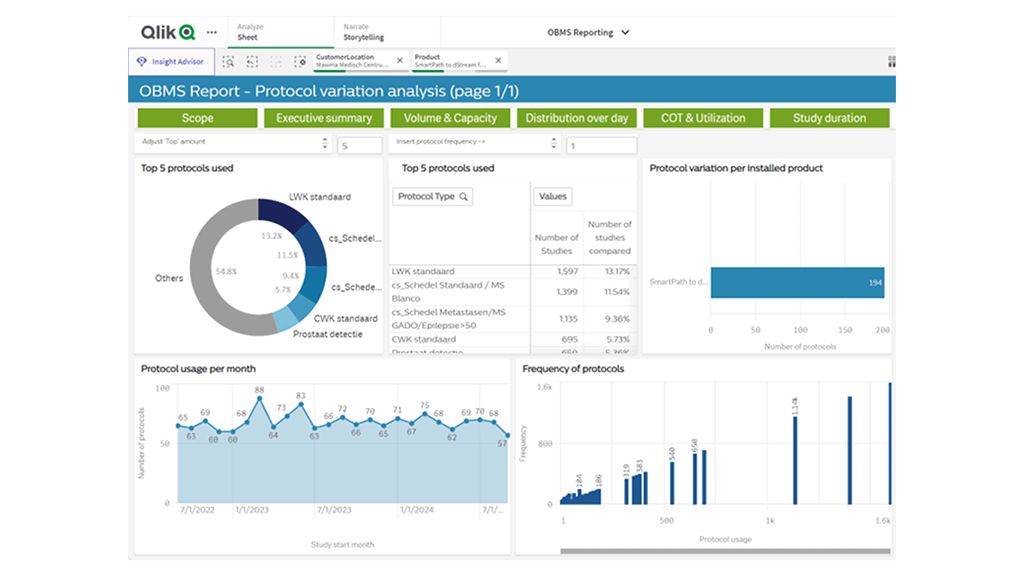
Example of data analytics dashboard displaying protocol variation analysis of one MR system
The Philips team conducted a thorough but brief qualitative analysis, surveying and interviewing staff of managers, radiologists, and MR operators to validate the quantitative findings and understand customer needs and process gaps. The results were combined with observations of examinations. This assessment provided input into some opportunities for improvement.
In the second phase of the project. Philips prepared an MR Value Stream map. This map diagrammed the patient pathway, from the MR request, performing the MRI exam, and finally the radiologist’s reports.
Some challenges were identified and mapped during a cross-functional stakeholder meeting. Possible efficiencies were identified and discussed. The Máxima MC team prioritized and selected strategies that could be implemented with consideration to the impact on patient care and the pilot timelines.
The efficiencies that were chosen were:
1. Improve patient care by ensuring the MR images are sent to PACS.
2. Optimize protocols to support confidence in diagnosis:
a. Improve image quality that support radiologists to provide good diagnostic reports.'
b. Improve workflow and communication between radiologists and MR operators.
3. Improve communication with other departments to reduce the delays in the inpatient flow.

Collaboration is key. Challenges were identified and mapped during a cross-functional onsite stakeholder meeting, discussing the patient’s value stream map, performing gap and root-cause analysis, prioritization, and designing solutions
1. Improve patient care by ensuring images are available on PACS
During the qualitative assessment, the neuroradiologist, Mark van der Vlies, MD, indicated that images were missing from the patient examinations. This occurs at least twice a day. Sometimes this omission was detected by the radiologist during their diagnostic reporting activities. The result was frustration and time loss of 3-5 minutes; the time needed to call the MR operators and get the missing images uploaded to PACS.
After discussion, the root cause of the missing images in PACS was found to be two-fold:
• The automated transfer functionality was not utilized
• The exam workflow might vary based on procedure or patient dynamics.
Implementing the change
To ensure that all exam images were sent to PACS, auto-image transfer was implemented on the individual MR scans in the protocols. This change was first implemented with neuro protocols. This allowed the team to validate this solution before adding the functionality to all protocols and MR systems.
As a result, all marked and acquired scans were sent to PACS automatically, including scans with patient motion and non-diagnostic scans. MR operators had perceived these non-diagnostic images in PACS as a disadvantage. However, the team agreed that the assurance that all scans were included in PACS was more important to patient care, and this strategy was therefore accepted.
An unexpected advantage was that radiologists could see the additional scans that were acquired to address image quality degradation or patient or physiological motion.
As a result of this implementation, all images are automatically sent to PACS and available for diagnosis, reducing the risk of misdiagnosis or delayed diagnoses due to missing images. In addition, the average number of calls regarding missing images was reduced from 2 to 0 per day, as measured by the neuroradiologist. This gives the radiologist an extra 3-5 minutes per day while reducing frustration.
I am happily surprised by the impact of the service. Philips acted as a middleman to improve the collaboration, scan protocols, and image transfer.

2. Optimizing protocols
Protocol optimization is a continuous process for all MR radiology departments. From the quantitative analysis conducted at Máxima MC, the system and software utilization were good. However, in the qualitative surveys, radiologists and MR operators recommended optimizing image quality.
From the surveys and interviews, the Philips and Máxima MC team also learned that the protocol optimization process, frequency, and scope were inconsistent across every domain Therefore, this pillar was split up into two implementation goals:
• Protocol optimization enabled by customized education, which is another Philips education offering.
• Workflow and communication between radiologists and MR operators.
MSK radiologist Elise Rasenberg, MD, was involved in the Clinical Advisory Services engagement with a focus on improving image quality and workflow efficiency in the radiology department. Elise emphasized the need for continuous improvement of image quality and workflow due to the high workload. She appreciated the support from Philips in optimizing protocols and highlighted the importance of ongoing collaboration to sustain progress and empower MR operators.
As part of the qualitative survey, the areas of image quality improvement were identified. Those were confirmed during interviews and image review sessions with radiologists.
Education
A two-day customized offsite training session was provided at the Philips Academy, Best, the Netherlands. During this session, key MR operators optimized the 1.5T protocols and discussed optimization approaches.
After the training event, Philips delivered a report to the radiologists and MR coordinator during their weekly radiologists meeting “Heilig uur”. Image optimization results were shared, and validation of the new protocols was planned.
The Máxima MC team tested the protocols in the clinical environment. Twelve new protocols were implemented on two 1.5T MR scanners. Six optimized protocols were implemented on the 3.0T system.
To evaluate the optimized protocols, a 5-point scale was created to assess signal-to-noise, contrast-to-noise, sharpness/resolution, and artifact level. The radiologist reviewed several patient cases before and after optimization and scored the image quality. The average scores are displayed in figure 1.
![Figure 1. Images displayed comparing before [A, C, E, G] and after protocol optimization [B, D, F, H]. Scores in blue bar indicate average result before the optimization. Scores in green bar indicate the average IQ result after protocol optimization.](https://images.philips.com/is/image/philipsconsumer/03e032c9672340cd8edeb38c00d895f3?extend=0,0,-3,0&wid=1500&hei=844&fit=stretch,1&$jpglarge$)
Figure 1. Images displayed comparing before [A, C, E, G] and after protocol optimization [B, D, F, H]. Scores in blue bar indicate average result before the optimization. Scores in green bar indicate the average IQ result after protocol optimization.
Improve workflow and communication
Based on feedback from interviews, there was a need for a good strategy for collaboration amongst radiologists and MR operators. Philips hosted a discussion with radiologists to discuss communication and expectations. The Máxima MC core team agreed upon a proposed approach. The new approach emphasizes clear and structured communication, well-defined expectations, the prevention of data overload, and taking end-to-end responsibility. These principles were then translated into actionable strategies.
Together with the radiologists, the key MR operators implemented this new way of working when optimizing their MSK MR protocols. This collaboration led to enhanced teamwork and satisfaction, greater confidence and ownership among key MR operators, and ultimately improved patient care through the delivery of optimized imaging.
We learned to understand each other better and have grown in confidence. One should actually not sell a product without this form of advisory.

3. Improve communication with other departments
Improve communication with other departments to reduce the delays in the inpatient flow.
During the observation days, the Philips team noticed that the examination workflow for inpatients had many dynamics, which could add challenges to the exam workflow. The teams noticed that inpatients were not always prepared for the MR exam and may not have received safety screening. This resulted in gaps and delays in the MR schedule because this critical screening needed to be done after the patient arrived at the MRI suite.
To address this, the MR team collaborated with other clinical departments to improve patient preparation. As a result, the department reduced delays and scheduling gaps and ultimately improved daily patient throughput.
The team introduced a communication step that successfully reduced system idle time during the day shift. This additional step involves a phone call from the MR department to the clinical department to communicate details about the upcoming inpatient’s MR exam, including preparation requirements and the expected schedule. Enhancing the scheduling process is regarded as a key factor in improving the daily experience for patients, MR operators, and medical staff.
The MR coordinator, Olaf van den Nieuwenhuijzen, indicated that the interaction between radiology, medical staff and patients is improved. The early interaction between nurses, patients, and radiographers led to timely informed patients and staff, and thus less frustration, fewer phone calls, re delays and fewer scheduling gaps.
Everyone benefits from using the rooms optimally. Data analytics in figures 2 and 3 show an improved system utilization of about 10% and a decreased change over time. The results can be translated as an increase of two additional examinations per day per system. The peaks are subscribed to flexibility in patient scheduling. Before the holiday period, open shifts are filled more effectively to cover the vacation time. Sometimes, during the holiday period, evening shifts can be cancelled. Are the peak periods experienced as intense? A period with many clinical patients was not perceived as particularly busy. The team seems to handle it easily.

Figure 2. Study volume per month measured from July 2024 to July 2025. Data includes two 1.5T and one 3.0T MR systems

Figure 3. Summary of data analysis and results. System utilization increased by more than 10%. Decreased average change over time. Average 2 more exams per day per system
Regular meetings were held to plan and support the implementation of the solutions and to follow up on the progress of each initiative. These meetings were attended by Philips consultants and the Máxima MC department staff. The team continues to monitor the quantitative and qualitative data available to ensure the implementation remains successful.
This Clinical Advisory Services engagement at Máxima Medical Center demonstrates the value of empowering clinical teams with analytics and expert support. By combining data-driven insights with collaborative problem-solving, the MR department achieved measurable improvements in efficiency, image quality, and team dynamics.
The neuroradiologist, Mark van der Vlies, M.D, was positively surprised by the contribution of the project to the optimization of protocols. Philips acted as a middleman improving the collaborations in specific clinical areas.
Head of radiology, Christel van Leeuwen highlighted the cultural and collaborative impact of the project, noting improved communication between radiologists and MR operators. She emphasized the value of structured advisory support and advocated for its integration into future system investments.
MR coordinator, Olaf van den Nieuwenhuijzen initially approached the project with skepticism but quickly recognized its value. He praised the hands-on collaboration, the educational sessions, and the improved mutual understanding between radiologists and MR operators. He also noted the workload challenges during implementation and the need for remote support tools.
Continued follow-up and structured advisory support are recommended to sustain and expand these gains.
Experience breakthrough innovation in 3T MRI with Philips' unique design
Explore Philips' 3T portfolio to boost clinical confidence with precision imaging for every patient, exam, and day using cutting-edge technology.

